Gum Disease
Services . Gum Disease
Maple Grove Dentistry
Gum Disease
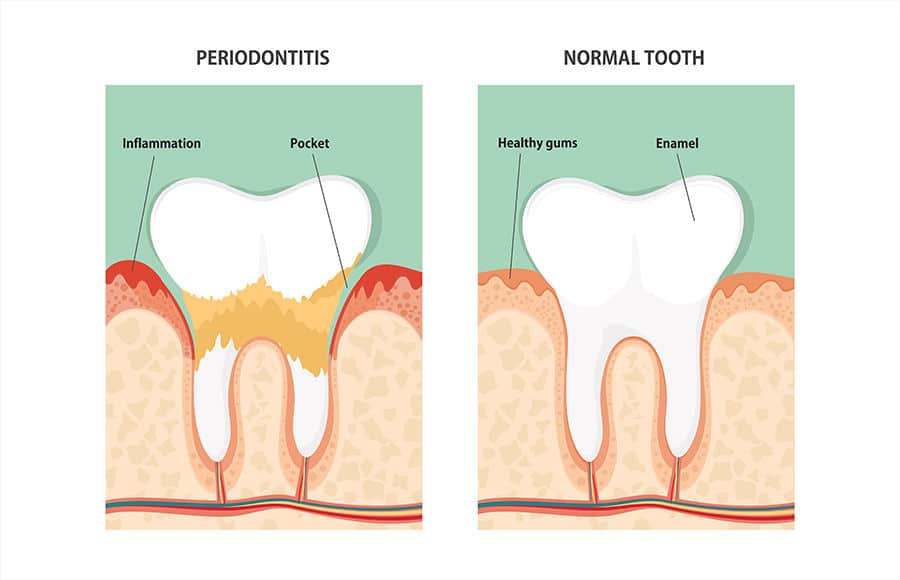
Gum Disease Diagnosis, Treatment, And Maintenance
Healthy teeth are the first thing we think of when we hear the term “oral health,” but healthy gums are just as critical as strong, cavity-free teeth. According to data from the Centers for Disease Control and Prevention, over 70% of Americans 65 years and older have some form of gum disease, either gingivitis or periodontitis. That’s a lot of people, but Dr. Jensen can help diagnose and treat the condition.
But it’s not just a concern for aging populations. Gum disease can affect anyone, at any age–man, woman, or child. With varying causes and characteristics, it truly behooves everyone to learn more about gum disease, including how it is (1) diagnosed, (2) treated, and (3) maintained.
If you think you may have gum disease, call Maple Grove Dentistry today to schedule your appointment with Dr. Jensen in our Boise, ID dental office.
About Gum Disease
If you’ve ever noticed your gums feeling puffy or swollen, seen blood in the sink after you brush/floss, or noticed your teeth feeling looser or looking longer than before—then take heed. You may be at risk for, or may already suffer from, gum disease. Educating yourself is the best way to be ready and know what to expect when you do eventually seek professional help. Even if you’ve never experienced any of the symptoms of gum disease, educating yourself is the best first step towards effective prevention.
Many causes of gum disease can be easily identified and prevented (inadequate dental care, tobacco use, poor nutrition), but some causes cannot be avoided—such as genetics, medications, or even stress. In other instances, gum disease may be an early indicator of another disease, or the result of a systemic illness, such as rheumatoid arthritis, diabetes, or cardiovascular disease. Hormonal changes in women can also contribute to the onset of gum disease.
Gingivitis And Periodontitis
Gum diseases fall into two categories, gingivitis and periodontitis. As the milder form, gingivitis is less severe, more easily reversible, and less permanently damaging. However, if gingivitis is left untreated, it can advance to periodontitis, a chronic inflammatory response that can cause permanent damage, such as loss of teeth, gum, and bone tissue.
While gums may not seem as important to you as your actual teeth, the truth is that you can lose both teeth and bone tissue if gum disease goes untreated. As inflamed gum tissue recedes from the base of your teeth, small pockets form, which can harbor bacteria and degrade the roots of otherwise healthy teeth.
The good news is that gum disease is incredibly treatable. For both types, there are surgical and non-surgical options to help stop, reverse and/or mitigate the damage. Even in the more severe cases, there are helpful treatments and reconstructive options available.
Diagnosing Gum Disease
If you suspect you might have symptoms of gum disease, a dentist or periodontist will conduct a comprehensive periodontal evaluation. This process looks at five factors to determine whether you are suffering from gum disease: teeth, plaque, gums, bite, bone structure, and risk factors. (A comprehensive periodontal evaluation checklist can be found here, if you would like to see the specifics.)
If you are experiencing any of the following symptoms, you’ll want to make an appointment with Dr. Russell Jenson to determine whether gum disease is the cause:
- Swollen, puffy, or shiny gums
- Bleeding when brushing or flossing
- Pain when biting or chewing
- Loose teeth, or a receding gum line on one or many teeth
- Bad breath, or a bad taste in your mouth
- A change in the alignment of your teeth
At your appointment, you can expect Dr. Jenson to ask you to describe both your symptoms and risk factors before conducting an exam. He will then look inside your mouth to check for visible symptoms and test your gums to see if they are quick to bleed when prodded.
Additionally, Dr. Jenson may use a dental instrument to check for the development of pockets in the space between your teeth and gums. This is an important step in the exam, as pockets greater than 3 millimeters can indicate gum disease.
You may also be asked to take a series of dental x-rays to determine whether you are experiencing bone loss at the sites of deeper pockets. Once the exam is complete, Dr. Jenson will discuss your diagnosis and the best course of treatment.
What Is The Treatment For Gum Disease?
After diagnosis, Dr. Jenson will recommend specific treatments for your teeth and gums. Some treatments involve medications, such as antibiotic mouthwashes administered at home, but most treatments will require special in-office or surgical procedures to reduce plaque and repair gums and tissue.
Not all procedures will be appropriate for every patient; be sure to ask questions to help you understand the doctor’s recommendations. You want to know what’s going on in your mouth before you start any treatment plan. If you don’t understand the diagnosis or recommendations, consider getting a second opinion before you proceed with treatments.
Some Non-Surgical Treatments Include:
- Scaling: during this procedure, dental instruments or ultrasonic devices (lasers) are used to remove tartar and bacteria from the surface of each tooth, both above and below the gum line.
- Root Planing: this procedure smooths the surface of a tooth’s root, to prevent further bacteria and tartar from lodging in the irregular surface of a damaged root.
- Antibiotics: some antibiotic treatments must be administered deep into the affected gum pockets, in the form of gels or slow-release chips or microspheres.
Some Surgical Treatments Include:
- Flap Surgery/pocket reduction surgery: this surgical procedure requires the gums to be cut and lifted back, exposing the tooth root to allow more efficient planning and scaling.
- Soft Tissue Grafts: when too much soft tissue in the gums is damaged, it can be helpful to use donor tissue (usually from your own soft palate) by attaching it to the damaged tissue. As it heals the graft provides greater coverage for the roots and prevents further damage.
- Bone Grafts: when periodontitis results in bone loss around the root of your tooth, it may be necessary to supplement with synthetic bone, donated bone, or small pieces of your own bone. The ultimate goal of a bone graft is to prevent loss of teeth, as more stable bones will hold your teeth more firmly in place.
- Guided Tissue Regeneration: as an alternative to bone grafting, this procedure actually clears the way and allows your body to regrow some of the bone that was destroyed by bacteria. Ask your Dr. Jenson for more information on the differences between guided tissue regeneration and bone grafts.
As you discuss these options with your dentist, ask questions and make sure you understand the recommended procedures and timeline. Keep in mind that all cases of gum disease are as unique as the teeth in your mouth. Some cases may be mild, but still require surgical procedures for correction. Other cases may be severe and widespread, needing several procedures to halt the damage to gums, teeth, and bone.
Long Term Maintenance
Most treatments for gum disease will require some after-care and home care, as your gums heal. Once your treatment plan is complete, there are distinct steps you will want to take to make sure your condition is under control and does not cause further damage.
Schedule Regular Dental Care
For many people, periodontal disease only develops because it wasn’t spotted in its early stages and prevented more vigilantly. However, once it develops it becomes a chronic condition, which can flare up periodically. The best thing you can do to keep your condition under control is to make sure you schedule regular dental visits for the future. Your dentist will recommend a schedule for check-ups and cleanings. These visits will help (a) prevent recurrence of gum disease by removing plaque and bacteria, and (b) spot flare-ups early.
Maintain a Home Dental Routine
Your goal at home is to keep bacteria and plaque build-up to a minimum, and your weapons are brushing, flossing, and using prescribed anti-bacterial rinses. All mouths are unique; if brushing/flossing twice a day wasn’t enough to prevent gum disease from affecting you, there’s no shame in admitting it might be time for a more assertive routine. You may need to start brushing after every meal, using a different type of toothbrush, or supplement your brushing with an interdental cleaner such as a Waterpik.
Medications
As with any medical procedure, the doctor will likely prescribe medications to help you heal and prevent further damage to your teeth and gums. As always, it’s important to follow instructions fully and for the required period of time. If you are told to use a prescription rinse indefinitely, don’t get lazy about refilling your prescriptions just because you are symptom-free at the moment. An attitude of “I’m healed, so now I can go back to my normal routine” is a dangerous trap to fall into.
Ultimately, gum disease can be a scary reality to face. As you get older you may already be thinking about the health of your gums as much as you think about the health of your teeth—but the reality is that gum disease can strike any person at any age. The best defenses are regular dental check-ups and arming yourself with the knowledge of both risk factors and the accessibility of effective treatments. When it comes to gum disease, it’s never too early to start educating yourself and it’s never too late to seek help from a periodontal professional.

